Feline hyperthyroidism at a glanceAbout: Feline hyperthyroidism is a common disease caused by a benign hormone-secreting tumour of the thyroid gland. Symptoms:
Treatment: There are several treatment options, including surgery to remove the tumour, radioactive iodine treatment to destroy the tumour, prescription diet or medications to control it. |
What is hyperthyroidism?
Also known as thyrotoxicosis, hyperthyroidism (FHT) is an endocrine (hormonal) disorder that is caused by the overactivity of the thyroid gland due to a benign tumour that speeds up your cat’s metabolism.
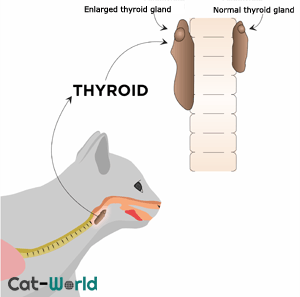
Located in the neck on either side of the windpipe, the thyroid gland produces two hormones, T3 triiodothyronine and T4 thyroxine, both of which control metabolism. Feline hyperthyroidism is the most common disease of the endocrine system, and according to the AAFC (American Association of Feline Practitioners, between 1.5 – 11.4% of cats globally have hyperthyroidism.
The most common cause is a benign tumour (adenoma) on one or both of the thyroid glands. It can be bilateral (80%) or unilateral (20%).
Other less common causes of feline hyperthyroidism include over administration of thyroid hormones when treating hypothyroidism (underactive thyroid gland) or a cancerous tumour, (known as a thyroid adenocarcinoma) of the thyroid gland. Less than 2% of cats with hyperthyroidism have a malignant tumour.
Clinical signs
- Weight loss
- Increased appetite
- Palpable thyroid gland (goitre)
- Diarrhea
- Vomiting
- Increased thirst and urination
- Behavioural changes such as nervous/jittery behaviour, aggression, over-grooming and or bald patches, hyperactivity and increased vocalisation
- Rapid heartbeat (tachycardia)
- Rapid, shallow breathing (tachypnea)
- Poor coat condition, see photos
- Thickening of the claws
- Hypertension (high blood pressure)
Less common symptoms:
- Weakness
- Decreased appetite
Diagnosis
The veterinarian will perform a physical examination which may reveal enlargement of the thyroid gland, elevated heart rate and weight loss. A diagnostic workup will be necessary to confirm the cat has hyperthyroidism.
- Baseline tests: Biochemical profile, complete blood count, and urinalysis to determine the overall health of your cat. Cats with hyperthyroidism may also have elevated liver enzymes.
- T3 and T4 tests: Specific blood tests to detect elevated levels of the hormones T3 and T4. Some cats with hyperthyroidism may show normal levels of these hormones in their blood test. If this is the case, your veterinarian will recommend a T3 suppression test. This involves a blood test to check the levels of T3 and T4, followed by the administration of oral doses of the thyroid hormone T3 followed by a second blood test. In a healthy cat, the level of T4 will drop, in a cat with hyperthyroidism the T4 levels will stay the same or increase slightly.
- Imaging studies: Thyroid imaging to evaluate the shape and size of the thyroid gland.
Hyperthyroidism classification
In 2016, the AAFP issued updated guidelines for classifying hyperthyroidism in cats as follows.
| Classic clinical disease | The cat has clinical signs of the disease along with an elevated serum total thyroxine concentration. |
| Possible hyperthyroidism with possible nonthyroidal disease |
The cat has clinical signs of the disease but a normal serum total thyroxine concentration. |
| Enlarged thyroid without clinical hyperthyroidism | The thyroid is enlarged, but there are no clinical signs and a normal serum total thyroxine concentration. |
| Subclinical hyperthyroidism | The cat has no clinical signs of disease but has an elevated serum total thyroxine concentration. |
| Clinical hyperthyroidism with confirmed nonthyroidal disease | The cat has clinical signs of the disease along with an elevated serum total thyroxine concentration AND confirmed concurrent disease(s). |
| Clinically normal | The cat has no clinical signs of the disease or enlarged thyroid but has an elevated serum total thyroxine concentration. |
Effects of hyperthyroidism on the cat
An increase in levels of thyroid hormones speeds up the cat’s metabolism (hypermetabolic state) which leads to a hyperdynamic cardiovascular state in which the heart beats faster which eventually causes congestive heart failure and secondary hypertrophic cardiomyopathy.
High blood pressure (hypertension) is another common side effect of hyperthyroidism in cats. Hypertension has a serious impact on several organ functions. Swelling and bleeding in the eyes can lead to blindness, hardening of the arteries, and a hardening of the heart muscle, which over time can cause congestive heart failure and increased risk of stroke.
Treatment
There are four options to treat hyperthyroidism in cats, and each treatment has its pros and cons. Treatment will depend on other medical conditions your cat may have as well as the availability of a nuclear medicine facility and cost. Kidney function must be evaluated before and after treatment as hyperthyroidism may mask chronic renal failure.
Diet: In 2012, Hills launched a prescription diet called Hills y/d to manage hyperthyroidism. This food is low in iodine, which is required by the thyroid gland to produce its hormones, low iodene=reduced hormone production. It can take a few weeks for this food to take effect.
- Pros: It is easy for the pet guardian to manage the disease and cheaper than surgery.
- Cons: It is not curative; it only manages the condition. Some cats may be reluctant to eat the diet or may go off their food when unwell, resulting in hyperthyroidism becoming worse again. Also, the thyroid tumour is still in the cat and may potentially turn cancerous in the future.
Update: I was recently contacted by somebody whose household cats were all put on Hills y/d as one of the cats had hyperthyroidism, and it was safest to feed all cats in the house the same diet. It would seem another cat had undiagnosed hyperthyroidism, and chronic kidney disease concurrently. The low iodine diet reversed the hyperthyroidism to the extent that the cat is now in severe kidney failure. Hyperthyroidism can protect the kidneys in cats with chronic kidney disease (see below) and great care must be taken when treating a cat who has both hyperthyroidism and kidney disease (I know first-hand because my cat died within two weeks of starting on hyperthyroid medication). I am not saying y/d is not a good product, but the lesson learned is if all cats in the household are to be fed y/d, test all cats for hyperthyroidism and kidney disease.
Drugs (Methimazole/Tapazole): The use of medication doesn’t cure hyperthyroidism, only control it. Medication is administered daily for the rest of the cat’s life. Short term this is the cheapest option, but in the long run, it can prove costly having to pay for daily medication for your cat. Methimazole can be given either in oral or transdermal (applied to the skin inside the ear) form.
- Pros: Treatment is reversible if side effects occur (see precaution at the end of this article).
- Side effects: Vomiting and lethargy.
Surgery: Removal of the enlarged thyroid lobe(s), known as a thyroidectomy.
- Pros: It is a permanent cure.
- Cons: Increased anaesthetic and surgical risks due to the effect the disease may have had on the cat’s heart and kidneys. If both glands are removed, there is an increased risk of accidentally removing the small parathyroid glands, (which among other things regulate the calcium supply in the body), which can cause hypocalcemia (low blood calcium).
If both lobes are removed, the cat will require daily thyroid supplementation.
Radioactive Iodine Treatment: The gold standard treatment for hyperthyroidism. A single injection of radioactive iodine (radioiodine I-131) concentrates in and destroys the diseased thyroid tissue while leaving the normal thyroid tissue intact.
- Pros: The cat doesn’t require anaesthesia, there is no need to give your cat medication for the rest of his life, and in the majority of cases, it is a permanent cure. Some cats will need to repeat treatment.
- Cons: It is expensive in the short term, and can only be performed at a specialist veterinary centre.
After treatment, the cat will be slightly radioactive and will have to stay in the hospital until radioactive levels drop to a safe level.
Hyperthyroidism and chronic kidney disease
For some cats, hyperthyroidism and kidney disease run concurrently. Hyperthyroidism can protect the kidneys because it produces a hyperdynamic cardiac state (increased blood flow). This increases glomerular blood flow (GBF) and glomerular filtration rate (GFR), which improves renal function.
Kidney failure can become worse once treatment begins and your veterinarian will recommend drugs or diet to control hyperthyroidism if your cat has concurrent kidney disease and closely monitor kidney function. That way, if the kidneys do begin to deteriorate the veterinarian can re-evaluate or stop the medication immediately, as opposed to surgery or radioactive iodine treatment which is permanent.
Why is hyperthyroidism on the increase in cats?
Hyperthyroidism was first described in 1979 and is now the most common endocrine disorder in cats. So why has this happened?
No specific breeds are prone to feline hyperthyroidism, although one research paper noted that Siamese and Himalayan cats are at a slightly lower risk of developing the disease.
Canned cat food
There has been research that points towards a link between the consumption of canned food and hyperthyroidism in cats, especially fish or liver flavoured varieties. BPA (bisphenol A) is a chemical used to line pet food cans to stop erosion and is a known endocrine disrupter, meaning it interferes with hormone systems. A large number of plastic products also contain BPA.
Polybrominated diphenyl ethers (PBDEs)
PBDEs are flame retardants that are known endocrine disrupters, which are found in many household products including furniture and electronic goods as well as in large fish.
Exposure occurs through inhalation of dust containing traces of PBDEs as well as ingestion during grooming or consuming a particular food. Several studies have found high levels of PBDEs in cats; however, no conclusive evidence shows a direct link between PBDEs and hyperthyroidism in cats. Certainly, there is a growing body of evidence towards the health risks of PBDEs.
Other
Lack of iodine supplementation in certain brands of cat food, but different reports suggest over-supplementation of iodine is the cause, exposure to well water, exposure to gas fireplaces, cat litter and frequent carpet cleaning. (Edinboro C.H. et al., 2004 and 2010). The general opinion is that it is likely several contributing factors that lead to hyperthyroidism.
Update December 2016. A study in the American Chemical Society’s Environmental Science and Technology journal points to fish flavoured food being responsible for exposing cats to PBDEs and PCBs.
Prevention
There is a foolproof way to prevent hyperthyroidism; certainly, exposure to tinned cat food, especially fish (which can contain high levels of iodine and PBDEs), and those with pop-tops seem to pose a higher risk to cats. Small cans are less likely to be lined with BPA.
- Use a natural cat litter with no scent.
- Avoid plastic food bowls and storage containers for pet food and water.
- Limit chemicals in the household environment, and switch to natural cleaning products as much as possible. See here for home-made, cat-friendly cleaners to use in the home.
- Install a water filter if possible to remove chemicals.
- Only heat food in glass or ceramic containers, not plastic.
- Routinely test all cats over the age of nine for hyperthyroidism during their annual exam.

