At a glance
|
Cat Health Collection
Cat health articles. Browse our health collection for common and uncommon cat health issues.
Hemophilia in Cats
Hemophilia at a glance
|
Asthma (Bronchial Disease) in Cats
At a glance
|
Feline Odontic Resorptive Lesions (Cavities) in Cats
What is a feline odontic resorptive lesion?
Also known as tooth resorptive lesions or cervical line lesions, feline odontoclastic resorptive lesions (FORL) is a common dental disorder in which odontoclasts (specialist cells responsible for reabsorbing the roots of deciduous or baby teeth) are reactivated and reabsorb the adult roots of the tooth. FORL occurs in between 20-75% of cats, the cause is unknown.
Lipomas in Cats
What are lipomas?
Lipomas are slow-growing, benign (non-cancerous) tumours of the fat cells that are surrounded by a fibrous capsule. They are quite rare in cats, and when they do occur, it is usually in older cats.
Broken Jaw in Cats
The jaw is one of the most common bone breakages to occur in cats. Most broken jaws occur as a result of a serious trauma such as a car accident, gunshot wound, kick or a fall from a height, resulting in the cat smashing his jaw on the ground. Bone cancer, bone infection, hyperparathyroidism and gum disease can all weaken the bones, leading to a broken jaw.
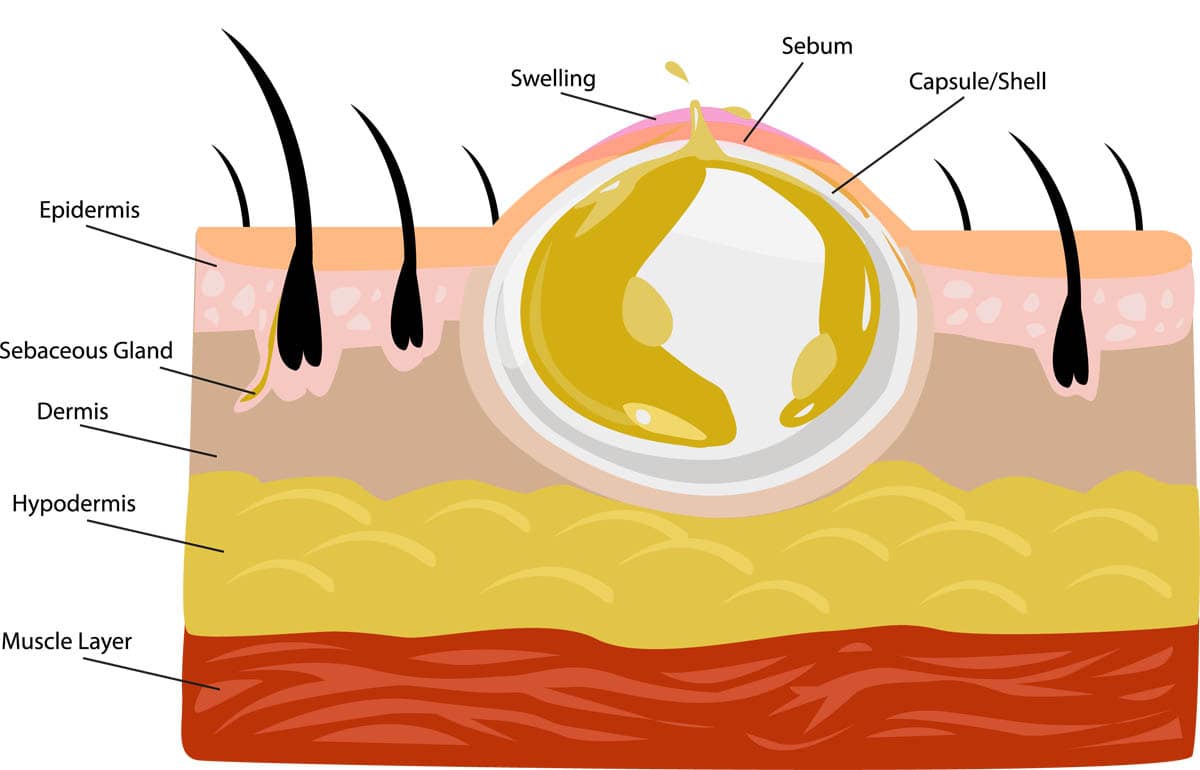
Sebaceous Cysts in Cats
What is a sebaceous cyst?
Sebaceous cysts (epidermal inclusion cysts) are benign tumours of the skin. They are the most common surface tumour found in cats and are composed of a thick, cheesy, yellow substance known as sebum, which is a secretion of the sebaceous gland comprised of fat and cellular debris, which lubricates and protects the skin.
Swollen Chin In Cats
Lumps under the cat’s chin may include bumps, masses and swelling along the jawline or underneath the lips. More than one lump may develop in some cats.
Most lumps under the chin are harmless, however, some can be potentially serious.
Skin Scraping Test in Cats
What is a skin scraping test?
A skin scraping test is a diagnostic test to determine the cause of almost all skin disorders in cats.
Many possible skin problems can affect cats, including fungal infections, parasites, inflammation, infections, cancer and allergies. Skin scraping tests can help determine the cause of the skin problem, confirm the presence of inflammatory cells, cancerous cells, bacteria, skin parasites such as mites, parasite eggs, fungi etc.