What is fatty liver disease?
Also known as hepatic lipidosis, fatty liver disease is the most common cause of liver disease in cats in North America and is associated with anorexia (loss of appetite). Starvation mode triggers the body to use fat (triglycerides) as fuel, which is sent to the liver to be processed into lipoproteins for energy. However, the cat’s liver is not very good at processing fat, and it begins to accumulate in the liver cells (hepatocytes), overwhelming it and interfering with its ability to perform many complex functions.
When the liver is unable to function as it should a cascade of derangements follow, which includes coagulopathies (bleeding disorders) and electrolyte imbalances.
There are two forms of hepatic lipidosis, primary or secondary;
- Primary hepatic lipidosis (idiopathic hepatic lipidosis) – No obvious medical cause. Middle-aged and obese cats are at the most significant risk. Stress is a major contributing factor to cats becoming anorexic.
- Secondary hepatic lipidosis – This form of hepatic lipidosis is due to underlying conditions such as diabetes, inflammatory bowel disease, cancer, enteritis, pyometra, cholangiohepatitis, pancreatitis and kidney disease, which causes a loss of appetite. Non-medical causes include stress such as a new animal in the home, stay at a boarding facility, accidental confinement or a weight-restricted diet.
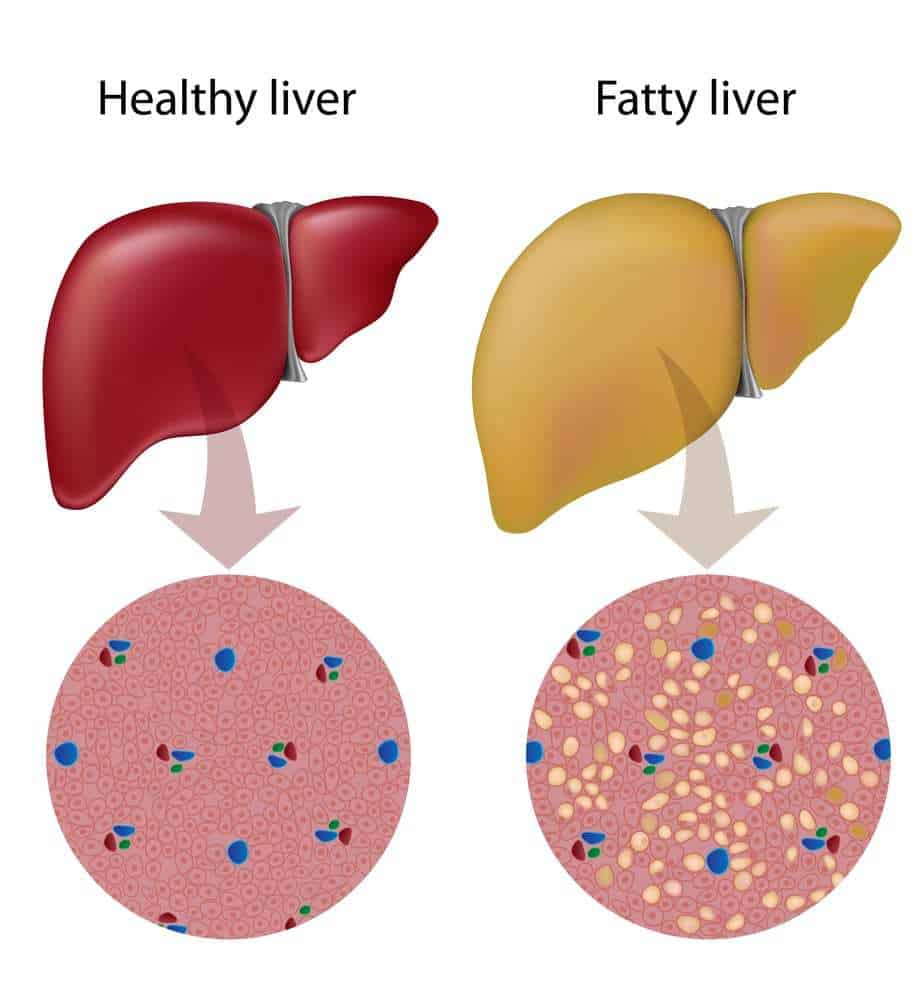
Symptoms of fatty liver disease in cats
In the early stages, there may be no signs of hepatic lipidosis other than anorexia, which highlights the importance that cat owners are aware of their cat’s eating habits and seek medical advice urgently if your cat stops eating.
- Loss of appetite (anorexia) for seven days or longer
- Weight loss
- Muscle wasting
- Dehydration
- Vomiting
- Excess drooling (due to nausea)
- Depression
- Lethargy
- Jaundice (yellow colour of the skin and mucous membranes)
- Unkempt coat
How is fatty liver disease diagnosed?
The veterinarian will perform a physical examination of the cat and obtain a medical history from you, which will include the onset of symptoms. During the evaluation, the veterinarian may feel the enlarged liver as well as icterus (jaundice), unkempt coat and dehydration.
Diagnostic workup:
- Biochemical profile: Will reveal increased ALP enzyme levels, as well as elevated bilirubin (bilirubinemia), in addition, electrolyte derangements can include hypokalemia (low blood potassium) due to loss of appetite, hypochloremia (low blood chloride) from vomiting.
- Imaging studies: Liver ultrasound or x-ray will reveal diffusely hyperechoic liver (the liver is brighter or more echoic than the spleen) and hepatomegaly (enlargement of the liver).
- Complete blood count: To look for destruction of red blood cells (hemolysis) and abnormal sized red blood cells (poikilocytosis) and non-regenerative anemia.
- Biopsy or fine needle aspirate and cytology: This will reveal liver cells that are swollen with lipid. A biopsy is not recommended for all cats as they are at increased risk of anesthesia and bleeding due to impaired liver function and should only be performed once coagulation factors and electrolyte abnormalities are corrected.
Treatment
One hospital reported a survival rate of 85% if the cat survived the first 96 hours; the prognosis is poor for cats who don’t receive prompt treatment.
Treatment depends on the severity of the disease and any underlying medical conditions. Aggressive nutritional support is necessary to save the cat and the prognosis is poor until the cat is voluntarily eating on its own. It is also important to address the underlying problem which contributed to the cat’s loss of appetite.
Treatment occurs in two phases, stabilising the cat and long-term care.
Phase 1-Stabilising the cat (hospital care)
- Intensive nutritional support. Most frequently, this involves trickle (continual) a calorie-dense, high protein liquefied diet via a nasoesophegal (NE) tube, which will be placed on the day of admission.
- Anti-nausea (antiemetic) drugs: Metoclopramide, maropitant to control nausea and vomiting.
- Fluid and electrolyte therapy: To maintain hydration and correct electrolyte derangements.
- Antibiotics: Amoxicillin or cephalosporin.
- Vitamin K: To help promote normal blood clotting.
- Gastric protectants: Proton pump inhibitors, H2 antagonist (famotidine), sucralfate.
- Other supplements may include taurine and vitamin B-12, which can help stimulate the appetite.
Phase 2-Long term supportive care (at home)
- Most cats will go home with a feeding tube which will enable the owner to support the cat nutritionally until he can eat on his own. Warm food to body temperature before administration and clean the tube before and after every meal. During this time, offer the cat food to see if he will eat on his own. It can take around six weeks for the appetite to return to normal.
- Oral antibiotics for 2-4 weeks to support liver function.
Do not let obese cats who have recovered to gain additional weight. Weight loss will be necessary for cats who are still overweight, under the close supervision of your veterinarian.
Cats who have had hepatic lipidosis are at greater risk of developing it in the future, so owners need to be watchful for signs of anorexia.
Prevention
- Be aware of your cat’s eating habits, and if you notice your cat eating less or nothing at all seek veterinary advice immediately.
- Never put your cat on a diet without close veterinary supervision.
- Try to prevent obesity in your cat, under close veterinary supervision.

